
Why is the fight to defend living standards, public services and personal freedoms, and the fight against imperialism, one and the same? Inspired by NZCTU President Sandra Grey’s refrain that “peace is union business”, I gave this public talk last month at Te Herenga Waka—Victoria University of Wellington.

This article is a lightly edited transcript of a public talk delivered at Te Herenga Waka Victoria University of Wellington on Tuesday 28 April, 2026. The recorded audio and slides of the talk are available here.
Tēnā koutou,
Kei te mihi ahau ki te tīamana mō to kōrero.
Ko wai au e tū ake nei?
Nō Kōtirana ōku tūpuna.
Ko Cornwall tōku waka.
Nō Ōtepoti ahau;
Ko Ngāi Tahu te iwi mana whenua o korā.
E noho ana au ki Pōneke;
Ko Taranaki Whānui te iwi mana whenua o konei.
Ko ISO te rōpū.
Ko Brookes tōku whānau.
Ko Grant tōku ingoa.
Nō reira tēnā koutou katoa.
A Surging Discourse on Imperialism
The world is on fire. Bombs are falling, drones are buzzing, and missiles are exploding from Palestine to Iran, from Lebanon to Venezuela, Sudan and Ukraine. So it’s little wonder that discourse on “imperialism” has surged worldwide in 2026. Here’s an indicator: Google searches including the word “imperialism” have been on the rise again.
Once the preserve of fringe socialist publications, the term is now appearing in mainstream media headlines. We might not be too surprised to see it pop up in liberal media outlets like The Guardian, New York Times, or MS Now, or even in Le Monde and the New Yorker. But it’s also creeping into headlines in centrist and non-partisan media, like CNN and AP News. It’s seeping into pop culture, and local papers. And it’s now turning up in quite unexpected places: in the media mouthpieces dedicated to concealing or mystifying the crimes of imperialism – like far right Zionist newspapers, and the world’s largest Christian media network. It’s even making mainstream media headlines here in Aotearoa New Zealand.
But while there’s currently a lot of talk about imperialism in the media, there’s not a lot of clarity about what the word means. And without knowing what imperialism is, we can’t know how to fight it.
A “Handful of Tyrants”?
One school of thought, widely-reported in the media, was expressed in a homily delivered by Pope Leo in Cameroon. His message resonated because it articulates one widely-held view about the nature of imperialism. Pope Leo said:
billions of dollars are spent on killing and devastation, yet the resources needed for healing, education and restoration are nowhere to be found. Those who rob your land of its resources generally invest much of the profit in weapons, thus perpetuating an endless cycle of destabilization and death.
Insofar as it goes, there is little to disagree with in Pope Leo’s thumbnail sketch of the system he labelled “imperialist” two weeks earlier. But he went on, ascribing a root cause to this system of exploitation and killing. Imperialism, says the Pope, is the fault of “a handful of tyrants.” And so he called on his followers to fight imperialism, as follows:
Let us look into each other’s eyes: we are this immense people!… Thus, my beloved predecessor exhorted us to walk together, each of us according to our own vocation, stretching the boundaries of our communities, beginning with concrete efforts on the local level, in order to love our neighbor, whomever and wherever he or she may be. You are witnesses to this silent revolution!
We can call this a moral response to imperialism. But here’s the rub: Pope Leo’s words about “tyrants” were widely understood as referring to Trump and his inner circle. The belief that Trump is to blame for imperialism is widely held, and reflected in some of those recent media headlines. Yet every US president since the 19th century has waged imperialist war. Since 2001, US presidents have spent US$8 trillion bombing 10 countries and killing a million people. The costliest of these wars were in Iraq and Afghanistan, where 51 other governments also sent troops.
So the problem is not “a handful of tyrants”, and love for our neighbour on its own isn’t a strong enough force to fight imperialism.
A Policy Choice?
A second school of thought about the nature of imperialism is that it’s a type of foreign policy – an option that governments resort to when they can’t achieve negotiated objectives through diplomatic means. This belief is also a widely held view. It’s represented in Aotearoa above all by the Green Party. But for reasons best known to itself, the party studiously avoids actually using the term “imperialism”. In fact, there are only two instances of the word on the vast Green Party website – once in the maiden speech by former Green MP Golriz Ghahraman, and once in their full Tagata Moana Policy.
On the international Left, this school of thought is most clearly expressed by figures like Jeremy Corbyn. Speaking at the 2026 Latin America Conference, he said: “When I was Labour leader, I wanted to develop an entirely new foreign policy that broke with principles of domination and imperialism… One that forges a partnership of equals, based on co-operation and mutual respect.”
The way to fight imperialism, according to this widely-held view, is to elect politicians with policies ostensibly opposed to imperialism. We can call this reformist anti-imperialism.
The first problem with this school of thought is that the major parties in liberal democracies – whether it’s Democrats and Republicans in America, or National and Labour here – are united around imperialist foreign policy. There’s a widespread myth that Helen Clark’s Labour government didn’t take part in America’s war in Iraq. In fact, two thirds of New Zealand’s navy frigate fleet joined the war effort. She also put boots on the ground in Afghanistan in the service of US imperialism, where they stayed for 20 years, killing civilians at a cost of at least $350 million.
The second problem is that even if a party like the Greens do win an election one day, government control over foreign policy is actually an illusion. This was clearly demonstrated to Jeremy Corbyn. In 2015, a serving general in the British Army publicly threatened a mutiny to topple the Government if Corbyn became prime minister and implemented his policy of scrapping the UK’s nuclear arsenal or withdrawing from NATO.
Examples like this aren’t confined to Britain. When New Zealand prime minister David Lange caved to public pressure in 1985 and announced a ban on nuclear ships visiting our ports, commanders in the New Zealand Defence Force opposed this threat to the ANZUS military alliance with the United States. They worked with the Pentagon and government officials in Wellington to undermine Lange behind the scenes. Former Chiefs of Defence Staff publicly attacked his foreign policy. This was just a decade after Australia’s Labor prime minister, Gough Whitlam, was ousted for much the same reason in a bloodless coup with CIA involvement. The defence establishment and senior officials ultimately succeeded in keeping New Zealand and Australia in the orbit of US imperialism.
But while politicians are beholden to the state, their foreign policy is directed even more strongly by the business community. It’s taken as a given that foreign policy must serve the “national interest,” which means in practice the interests of capitalists such as exporters and the corporate sector.
So the third problem with the view that imperialism is a policy choice is that military action and diplomacy are two sides of the same coin. In Iran, bombing and diplomatic sanctions are symbiotic components of a unified American policy.
The politics and economics of imperialism are inseparable. Trade deals, military alliances, cooperation agreements, tariffs, supply chains, loans, international summits, financial bailouts, foreign investment decisions, overseas aid, and so on are all intrinsic parts of imperialism. Imperialism isn’t a policy choice. It’s a system.
Unipolar Imperialism?
The third and final school of thought I want to address is not such a widely-held view. But it’s significant for two reasons. Firstly, because it’s an ideological current in the anti-imperialist movement that ISO is part of. And secondly, because it claims to be Marxist.
This school of thought is represented internationally by scholars and commentators like Vijay Prashad, who did a speaking tour of Aotearoa in 2024, and Caitlin Johnstone, with her half-million followers on social media. But its pre-eminent representative in Aotearoa is Josephine Varghese, an activist and lecturer in political science at the University of Canterbury Te Whare Wānanga o Waitaha. Her professional biography describes her as “a public spirited academic with interests in geopolitical analyses using postcolonial and Marxist theories,” with particular expertise in imperialism. She is connected to the Canterbury Socialist Society and Palestine Solidarity Network Aotearoa, and is a regular contributor to the 1/200 Podcast and the Democracy Project based here at Te Herenga Waka Victoria University of Wellington.
Varghese goes beyond moral opposition to imperialism, and she understands imperialism as a system, not a government policy choice. “The imperial system,” she says, “is not only a military network (we are familiar with the military network). It is a financial network (e.g. IMF, World Bank), trade (WTO), information and media (e.g. Reuters, AFP, AP).” But she argues that:
while imperialism is linked to capitalism, these are not one and the same… Capitalism is the prevailing mode of production, but imperialism is slightly different. It is the system/network and set of processes which enforces capitalism across the world.
For this reason, Varghese says, “we have to see USA as a unique threat,” because the “United States is the seat of capitalism.” Varghese quotes Che Guevara in support of this view: “While envisaging the destruction of imperialism, it is necessary to identify its head, which is no other than the United States of America.”
By arguing that imperialism and capitalism “are not one and the same,” Varghese can divide capitalist countries into two camps: the imperialist camp, headed by the United States, and the anti-imperialist camp, made up of capitalist countries in opposition to the United States. We can call this school of thought campism. Varghese is explicit about which countries are supposedly anti-imperialist. “Russia has oligarchs,” she admits, “but Russia is not the seat of global capitalism… So this is the fundamental difference between the foreign policy of USA and Russia.” And, she adds, “if you think about China, China is not interested in enforcing capitalism across the world” either.
The problem with this school of thought is twofold.
Firstly, campism aligns the fight against imperialism with support for the governments of the supposedly anti-imperialist camp. Varghese is not squeamish about openly supporting dictators. She defends Libya’s Muammar Gaddafi as someone who “had universal education, universal healthcare,” and who “funded all sorts of freedom struggles all around the world.” She defends Vladimir Putin, claiming that in Ukraine “the aggressor is the United States.” She even defends Syria’s Bashar al-Assad as someone “no more dangerous than any Western leader.” She whitewashes the crimes these regimes commit against their own people. In Iran, she denied the government crackdown on protests at the start of 2026 ever happened: “The idea that the Iranian government is this powerful entity just killing its citizenry is mistaken.”
And secondly, campism denies the agency and democratic will of people who rise up against these dictators and autocrats. In Ukraine, Varghese smeared the 2014 popular uprising that toppled president Viktor Yanukovych. She compared the protesters with the anti-vax conspiracy theorists who occupied our own parliament grounds in 2022, claimed they were motivated by support for neoliberal ideas spread by the global media, and described their revolution as an anti-democratic “coup.”
Our Anti-Imperialism
Fortunately, the worldwide surge in Google searches that include the word “imperialism,” mentioned at the start of this talk, have focused on another school of thought. Here are the “related queries” people typed into Google:
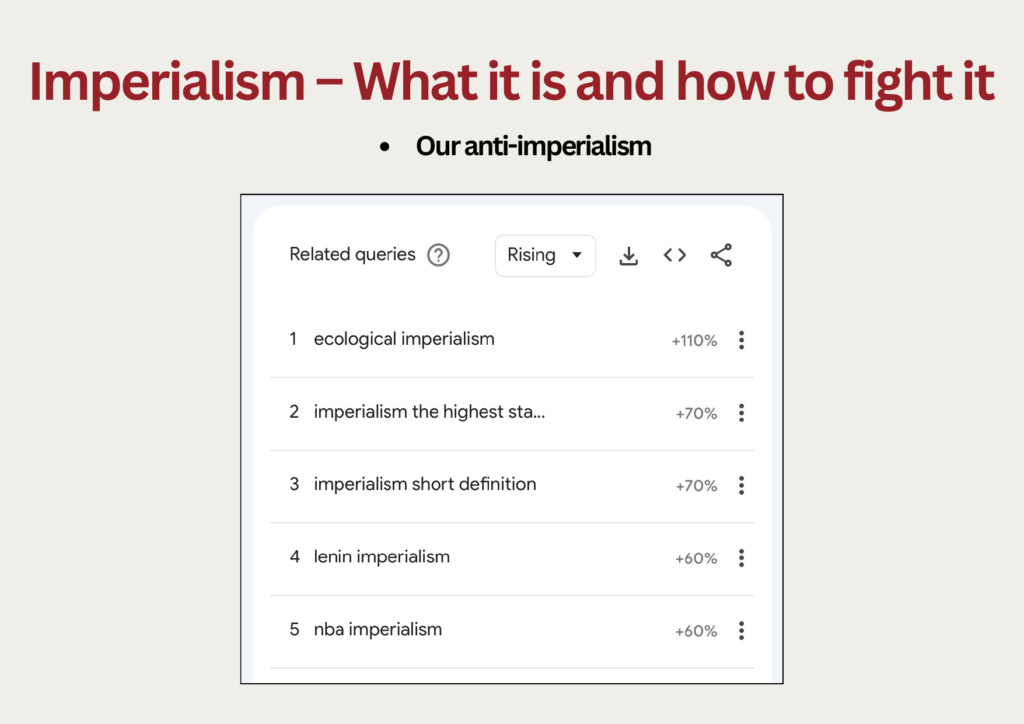
People are reading Lenin, who is also a reference point for our anti-imperialism in the ISO.
But before I get onto our own school of thought, I want to stress that moral opposition to imperialism, reformist opposition, and campist opposition all get some things right. Love for our neighbour, in Pope Leo’s sense, is a good thing. It’s part of forging real bonds of solidarity. Foreign policy that favours diplomacy is something we want. And although it’s for different reasons than the ones given by Varghese, which I’ll get into soon, she is right that our key focus must be opposing US imperialism. ISO marches alongside people from all three schools of thought.
Lenin, like Varghese, claims to be Marxist. But Lenin’s most-searched book, Imperialism, the Highest Stage of Capitalism, contradicts Varghese on key points. Where Varghese thinks that capitalism and imperialism are two different things, Lenin counters: “In its economic essence, imperialism is monopoly capitalism.”
We probably all have some idea what “capitalism” is. But what does Lenin mean by “monopoly capitalism”? In his introduction to a brilliant book by Nikolai Bukharin called Imperialism and World Economy, Lenin explains it this way:
There had been an epoch of a comparatively “peaceful capitalism,” when it had overcome feudalism in the advanced countries of Europe and was in a position to develop comparatively tranquilly and harmoniously, “peacefully” spreading over tremendous areas of still unoccupied lands, and of countries not yet finally drawn into the capitalist vortex.
Of course, even in that epoch, marked approximately by the years 1871 and 1914, “peaceful” capitalism created conditions of life that were very far from being really peaceful… For nine-tenths of the population of the advanced countries, for hundreds of millions of peoples in the colonies… this epoch was not one of “peace” but of oppression, tortures, horrors that seemed the more terrifying since they appeared to be without end.
We are all vividly aware of what this meant during the colonisation of Aotearoa, so we shouldn’t hold any romantic notions of this period. We merely understand that to have been a time when capitalist countries were able to enact some of their rivalries in less direct conflict with one another, by instead expanding to occupy non-capitalist regions. However, “This epoch has gone forever,” said Lenin:
It has been followed by a new epoch… this change was caused by nothing but the direct development, growth, continuation of the deep-seated and fundamental tendencies of capitalism and production of commodities in general.
The growth of commodity exchange, the growth of large-scale production are fundamental tendencies observable for centuries… At a certain stage in the development of exchange, at a certain stage in the growth of large-scale production, namely, at the stage that was reached approximately at the end of the nineteenth and the beginning of the twentieth centuries, commodity exchange had created such an internationalisation of economic relations, and such an internationalisation of capital, accompanied by such a vast increase in large-scale production, that free competition began to be replaced by monopoly. The prevailing types were no longer enterprises freely competing inside the country and through intercourse between countries, but monopoly alliances of entrepreneurs, trusts.
The typical ruler of the world became finance capital, a power that is peculiarly mobile and flexible, peculiarly intertwined at home and internationally, peculiarly devoid of individuality and divorced from the immediate processes of production, peculiarly easy to concentrate, a power that has already made peculiarly large strides on the road of concentration, so that literally several hundred billionaires and millionaires hold in their hands the fate of the whole world.
Lenin wrote this in 1915. We immediately recognise that the picture is the same today.
So fighting imperialism cannot be separated from the fight to end capitalism in its current stage of development. Or, as Lenin put it: “The reply of the proletariat to… imperialism… [must be] the abolition of capitalism.” Lenin did not say that the reply to imperialism must be the abolition of capitalism in America while continuing with capitalism in Russia, Iran, and China. To fight imperialism, we must stand with working people against their capitalist governments – in every country. Capitalist imperialism is a global system. In abolishing it globally, Marx himself declared: “the emancipation of the working classes must be conquered by the working classes themselves.” Imperialism cannot be conquered by Iranian missiles, nor by Putin’s tanks. It cannot be conquered (and I shudder that I have to make this point) by Assad’s barrel bombs and his indiscriminate use of chemical weapons against internal opponents.
At the same time, however, Lenin argued: “Imperialism is forcing the masses into this struggle by… worsening the conditions of the masses both economically – … [through the] high cost of living – and politically – [through the] growth of militarism, frequent wars… and colonial plunder. Victorious socialism must achieve complete democracy and, consequently… give effect to the right of oppressed nations to self-determination.” Defending the right to self-determination for oppressed nations, like Iran, means we resist all US attempts to impose regime change or dictate Iranian policy from without – whether through quick assassinations, or the slow pressure of military attrition, blockades or sanctions. Changing the repressive capitalist government in Tehran is a matter for the Iranian people themselves. In the current conflict, we hope Iran’s war of self-defence is successful.
In Ukraine, it is true – as Varghese and others point out – that the US is (in her words) “meddling in Ukraine sovereignty.” But that doesn’t mean defending Russia’s imperial conquest. As Lenin said, “The fact that the struggle for national liberation against one imperialist power may, under certain circumstances, be utilised by another “Great” Power in its equally imperialist interests should have no more weight in inducing Social Democracy [socialism] to renounce its recognition of the right of nations to self-determination.” He was even talking about self-determination for Ukraine in this article, 110 years ago. ISO supports the Ukrainian right to self-determination and we oppose Russian and American imperialism alike.
What Is To Be Done?
So if this is the nature of imperialism, how do we fight it here and now in Aotearoa?
Over the last century, theorists and activists within the broad Leninist school of thought have debated and tweaked how they fought imperialism in response to changing circumstances; so no single line from the past can be taken as gospel. Having said that, fellow Bolshevik Leon Trotsky once put it this way: “The struggle of the proletariat against war is the continuation and sharpening of its class struggle… In this struggle the basic principle is: “the chief enemy is in your own country,” or “the defeat of your own (imperialist) government is the lesser evil.”
Our government is a junior partner in the imperialist bloc headed by the United States. This has been true under both National and Labour administrations. It’s for this reason that a key focus for us is fighting US imperialism. Christopher Luxon has openly called for the New Zealand military to become “a force multiplier for Australia and the US and other partners.” Last year, 700 New Zealand troops took part in the Talisman Sabre exercise. RNZ reported: “Talisman Sabre aligns with US efforts to build a vast network of sensors and shooters across the Indo-Pacific… The New Zealand Defence Force said a key goal is to be able to integrate its capabilities into Australian and US command relationships.” To create this “force multiplier” for Washington, Luxon’s government plans to double military spending by 2029 at a cost of $12 billion. At the same time, it’s cutting $12 billion in pay equity funding, starving hospitals and slashing the Climate Emergency Response Fund. The fight against imperialism and the fight to defend public services and our standard of living as workers are one and the same.
New Zealand is also a member of the Five Eyes intelligence-sharing network, headed by the United States. Two weeks into the war on Iran, Foreign Minister Winston Peters and Defence Minister Judith Collins called this network “vital to security” and singled out Iran as the threat. The Five Eyes network provides the Pentagon with targets for military strikes. It also gives US agencies such as ICE access to our biometric data when we travel there. The US is now demandingwholesale access to all biometric data held by the New Zealand government. The fight against imperialism, and the fight to protect ourselves from surveillance, detention or worse at the hands of shadowy US forces, are also one and the same.
This is to say nothing of government support for Rocket Lab. The Coalition has approved their launches of US military satellites from Māhia, after the company announced it was “ready to serve the US Department of Defense.” Rocket Lab has not denied that these satellites have been used in the bombing of Iran. Rocket Lab is also working for the Israeli military.
In the current war of choice against Iran, which is increasing financial pressures on workers both here and overseas, we raise the working class demand for peace. At the same time, we recognise that an outcome which favours Iran would clearly be the “lesser evil” for working people in Aotearoa. An outcome which strengthens Trump, and boosts Washington’s power to export their culture wars and privatisation agenda here and around the world, would be worse.
So what is imperialism? It’s capitalism in its current stage of development. How do we fight it? By sharpening class struggle, demanding an end to all military and intelligence ties between New Zealand and the US, and supporting working class struggles to defend living standards and the rights of oppressed peoples everywhere.
Nō reira, tēnā koutou, tēnā koutou, tēnā tātou katoa.
• First published by the International Socialist Organisation. Reposted with permission










